Prevention Alzheimer
6.1. STROKE AND CEREBRAL INFARCT IN LYME DISEASE
Meningovascular form of Lyme neuroborreliosis – a major form of chronic/late Lyme neuroborreliosis
Miklossy J, Kuntzer T, Bogousslavsky J, Regli F, Janzer RC. Meningovascular form of neuroborreliosis: Similarities between neuropathological findings in a case of Lyme disease and those occurring in tertiary neurosyphilis. Acta Neuropathol 1990;80:568-572.
Abstract
Recent observations have delineated the neurological manifestations of Lyme disease, but, to our knowledge, no detailed neuropathological study from autopsy cases has been reported. In this report we describe the neuropathological findings in a case of Lyme neuroborreliosis. The chronic meningitis, the occlusive meningovascular and secondary parenchymal changes that we found are similar to those occurring in the meningovascular form of neurosyphilis. Thus, we suggest that the case described here represents the meningovascular form of tertiary Lyme neuroborreliosis.
Kuntzer T, Bogousslavsky J, Miklossy J, Steck AJ, Janzer RC, Regli F. Borrelia rhombencephalomyelopathy. Arch Neurol 1991;48:832-836.
Abstract
Three patients, in whom the diagnosis of Borrelia burgdorferi infection was unknown for several years, developed a biphasic involvement of the central nervous system: an acute brain-stem dysfunction was followed up, in two patients, by a progressive, disabling myelitis and, in one patient, by further relapsing-remitting episodes of severe multifocal rhombencephalitis. The most consistent cerebrospinal fluid abnormalities in the analysis of sequential specimens were elevated total IgM levels that normalized after penicillin therapy. The neuropathologic findings in one patient showed microgliosis and meningovascular involvement of the central nervous system, resulting in two ischemic infarcts in the myelencephalon. Few spirochetes were localized in the leptomeninges and around subependymal vessels of the fourth ventricle. The vascular element consisted of an obliterative inflammatory vasculopathy in the medullary parenchyma. This study (1) provides pathologic evidence that a vascular disease induced by B burgdorferi is a pathogenetic mechanism for cerebrovascular diseases, and (2) emphasizes the similarities between neuroborreliosis and neurosyphilis.
Illustration of the first neuropathologically confirmed case of late or chronic meningovascular neuroborreliosis, which is the example of secondary parenchymatous tertiary form of the disease. – Chronic meningitis, Heubner’s arteritis and secondary cerebral infarcts were observed at autopsy in a patients with clinically and serologically confirmed Lyme neuroborreliosis (Miklossy et al., 1990, Kuntzer et al., 1991).
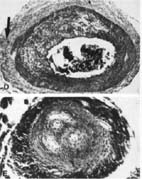
Illustration of the first neuropathologically confirmed case of late or chronic meningovascular neuroborreliosis, which is the example of secondary parenchymatous tertiary form of the disease. – Chronic meningitis, Heubner’s arteritis and secondary cerebral infarcts were observed at autopsy in a patients with clinically and serologically confirmed Lyme neuroborreliosis (, Kuntzer et al., 1991).
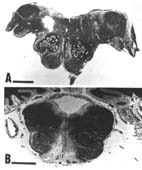
The diagnosis was based on the clinical and pathological findings, positive serology for Borrelia burgdorferi, intrathecal production of anti-Borrelia burgdorferi antibodies, and on the presence of silver-stained spirochetes morphologically compatible with Borrelia (Miklossy et al., 1990, Kuntzer et al., 1991).
These articles highlight that Borrelia burgdorferi similarly to Treponema pallidum can cause cerebral infarcts.
It is important to consider in the differential daiagnosis of cerebral infarcts that Borrelia burgdorferi can be responsible for a small percentage of the cases.